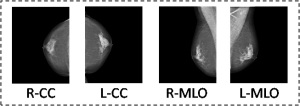
Using an AI program and analyses from
radiologists made a cohort of breast cancer
diagnoses approximately 90 percent accurate
Radiologists at NYU School of Medicine have collaborated with the NYU Center for Data Science to develop a new approach that results in a drop in the number of biopsies required to verify breast cancer diagnoses.
Researchers found that combining the pattern recognition capabilities of a machine learning computer program, trained on more than one million images, with analyses performed by radiologists yielded approximately 90 percent accuracy in diagnoses. The aim is to raise the confidence of physicians in assessments made for mammograms, so that biopsies do not need to take place as much.
“The radiologists alone achieved an accuracy of 0.78 on average. The neural network alone achieves approximately an accuracy of 0.87. A hybrid model (one radiologist plus a neural network) achieves approximately 0.89 accuracy on average,” senior study author Krzysztof J. Geras, assistant professor in the department of radiology at NYU Langone and an affiliated faculty member at the NYU Center for Data Science told HCB News. “When all of the radiologists teamed up together with the model they achieved 0.91 accuracy.”



Ad Statistics
Times Displayed: 2839
Times Visited: 27 Fast-moving cardiac structures have a big impact on imaging. Fujifilm’s SCENARIA View premium performance CT brings solutions to address motion in Coronary CTA while delivering unique dose saving and workflow increasing benefits.
More than 39 million mammograms were performed across the U.S. on women who showed no symptoms for breast cancer to determine those who required closer follow-up. Those who showed abnormal mammogram findings were referred for biopsies.
The approach by the team combines the ability of AI to detect pixel-level changes in tissue invisible to the human eye with forms of reasoning possessed by the radiologist but not AI. Together, the two are meant to decrease the occurrence of false-positives and false-negatives, thereby raising the confidence of the physician.
Researchers deployed statistical techniques within their program that enabled it to "learn" which image features increase prediction accuracy as it reviews more and more data, rather than being told how to by individuals. The program was trained on a database of 229,426 digital screening mammography exams and 1,001,093 images analyzed by the researchers and collected over seven years by NYU Langone Health in routine clinical care. The images were correlated with biopsy results, enabling the researchers to program the neural network with scans for which cancer diagnoses were already determined. Its accuracy was measured by the number of correct predictions it made.
They then tested the ability of the program to add value to the diagnoses of 720 mammogram images reviewed by 14 radiologists. The program did so by first assessing the very small patches of the full resolution image separately to create a heat map to determine statistical likelihood of disease. It then evaluated the entire breast for structural features linked to cancer, correlating its findings with those it flagged in the pixel-level heat map.
Geras says the team plans to build upon the accuracy of the program by feeding it more data, possibly to the point where it may be able to identify changes in breast tissues that have not yet become cancerous but have the potential. Though they are not currently training the program for screenings of other forms of cancer, Geras says this too could happen at some point.
“This is definitely possible and I'm sure many groups will soon show very similar results with cancers in other body parts,” he said.
The findings were published in the journal,
IEEE Transactions on Medical Imaging.

